Ms. Julia Achen woke up after general anesthesia for back surgery with a very sore throat. The discomfort persisted for about three months. Her voice was also hoarse immediately upon awakening. Her vocal quality still remains poor. Some days her volume is reduced to a whisper. She can no longer sing in her upper range. Her voice gives out or it cuts in and out during use. She can no longer yell loudly. When she first inquired about her voice problems, her surgeon said, “Given the size of your mouth, it might’ve been a difficult intubation, but most times these problems resolve on their own.”
The surgeon was assuming that the anesthesiologist somehow rubbed the vocal cords when putting the endotracheal tube in, perhaps causing swelling. She did not improve and eventually, she saw an ENT. Initially he suggested that her problem might be from acid reflux. On a follow-up exam, he thought one of the arytenoids may have been dislocated when the anesthesiologist was trying to insert the breathing tube. When I saw her, the right vocal cord was much looser than the left, which allowed air to leak out the right side. It appeared to me that her right vocal cord had been torn during the intubation and had healed with less tension. There was also a small white deposit within the vocal cord, at the back edge.
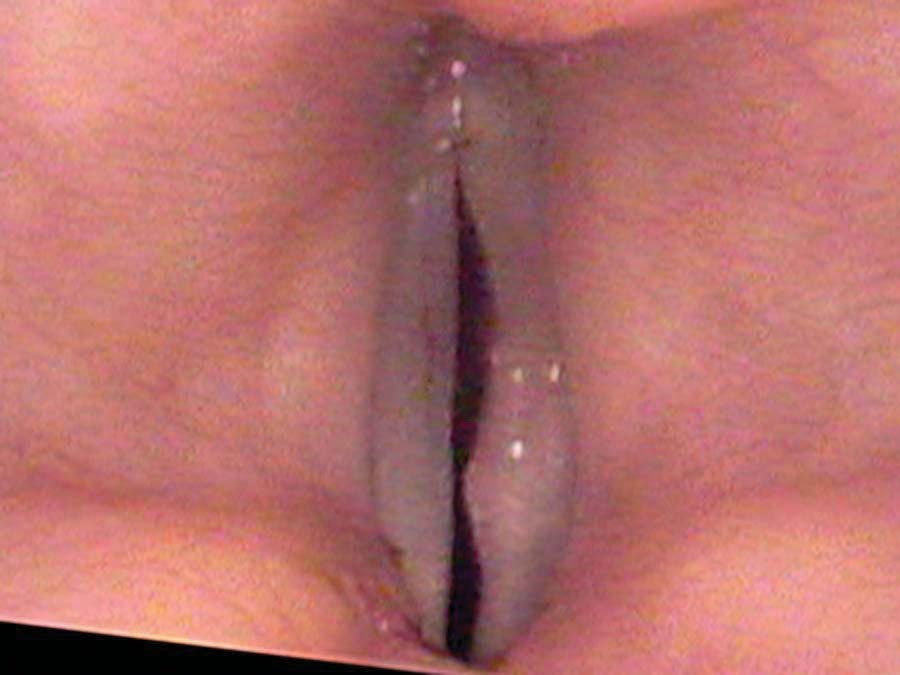
Singers, who are basically vocal athletes, notice these types of limitations more than regular speakers. Although some injuries can be improved upon, other injuries may not be correctable. The better care would be to learn how to avoid injuring the larynx.
I encourage anesthesiologists and surgeons to refer everyone with a hoarse voice after surgery, not only for the patient’s benefit, but for the physician to learn what complication he may have had. My experience is that most physicians, including surgeons and anesthesiologists, have a tendency to tell people with a hoarse voice after surgery that they will get better. While most do, many individuals after surgery have some ongoing voice limitation and anesthesiologists and surgeons do not learn about the problems they cause when they ignore them, so their technique is never modified.
Intubation Granuloma and Granulomas of Healing
When asleep under anesthesia, the endotracheal tube puts pressure on the vocal cords near the vocal process. The cartilage is just below the surface and the mucosa overlying the cartilage is easily injured just from pressure. This is one mechanism for the formation of a contact granuloma — a reactive healing response to mucosal injury at the vocal process.
Granulomas can occur anywhere the mucosal lining has been left open to the bacteria of the throat. They may occur on a surgical site or on an overuse ulcer. The treatment for granulomas of healing is similar to those of overuse — identification and correction of the underlying irritant, whether it is contact pressure, reflux, or voice misuse.
Stripping
Prior to the development of delicate instruments, lasers, and techniques to remove tiny bumps from the vocal cords that we now have available, there was a basic instrument called the cup forceps. The technique evolved into grabbing the nodule in the forceps, twisting, then pulling, stripping or yanking the nodule off. If you were lucky, just the nodule was removed. Far more often a long strip of mucosa ripped off. Too often the surgeon also grabbed too deeply and tore off not only the nodule and some of the surface tissue, but the lubricating layer of the vocal cord as well.
New skin grew over the injured area. If there was no nodule left and the edge healed straight, the voice could sound better. This apparent improvement resulted because this stripped cord was stiff enough now not to vibrate, so sound only came from the good cord — a bit like a person with double vision having one eye removed to improve the double vision. True, the double vision is gone, but there is not much reserve if there is a problem with the remaining good eye. Stripping is becoming less common, but there are a number of surgeons still performing the procedure.
What you learned
- An endotracheal tube can tear, dislocate, or compress the vocal cords during intubation — leading to cord asymmetry, reduced tension, and chronic hoarseness that does not resolve on its own.
- Patients with a hoarse voice after surgery should be referred for laryngoscopy rather than told to wait; physicians who do not follow up do not learn from their complications.
- An intubation granuloma forms when the tube presses on the mucosa overlying the vocal process cartilage, injuring it and triggering a reactive healing response.
- Vocal cord stripping — using cup forceps to yank off nodules — frequently removes the lubricating Reinke’s space layer along with the lesion, causing permanent stiffness.
- A stiff cord that no longer vibrates may superficially “improve” the voice by eliminating the double vibration — but this masks the damage rather than repairing it.
